Assessing the Risk of Acute Kidney Injury: A Paradigm Shift in Renal Care
Dr. V. Seenu Reddy, MD MBA, FACS, discusses the implications of NEPHROCHECK® Test [TIMP2 · IGFBP-7] to identify at-risk patients.
How can early identification of AKI affect patient outcomes?
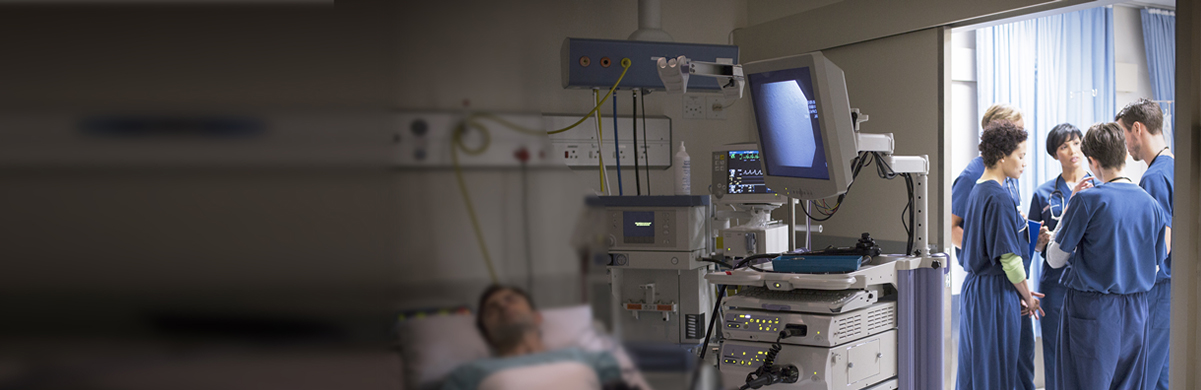
Dr. Jeffery Vender examines how new biomarkers could benefit patients by identifying their risk for acute kidney injury earlier. AKI is often recognized late and can result in morbidity, mortality and increased cost of care.
A Familiar Danger
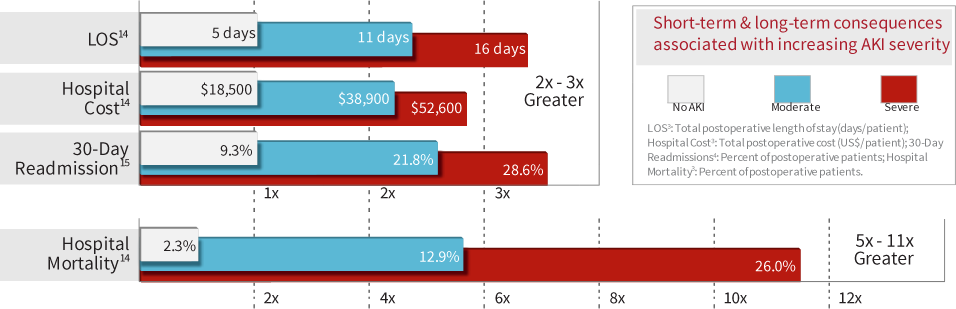
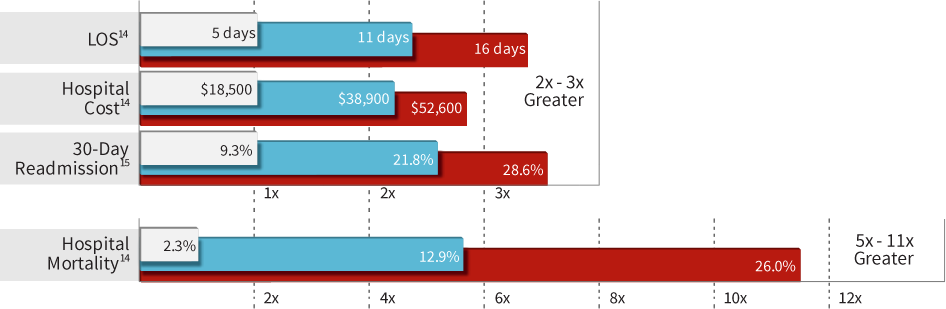
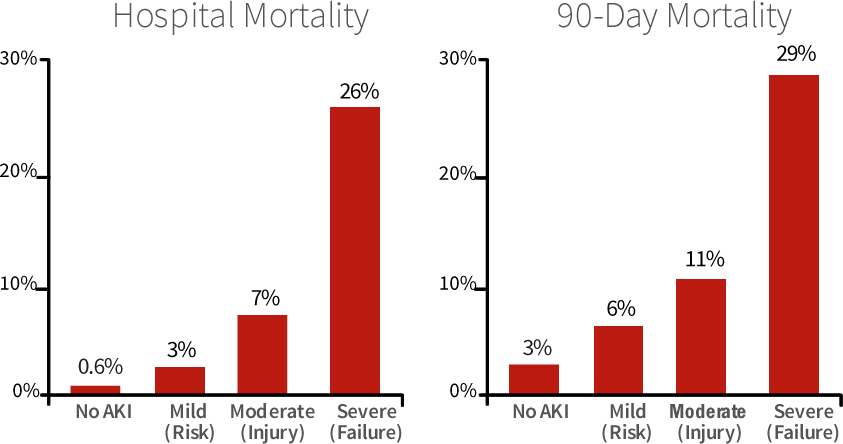
Acute kidney injury is an all too common complication, afflicting between 7 percent and 18 percent of all hospitalized patients4 and up to 50 % of critically ill patients.5 The condition is associated with a 10-fold increase in hospital mortality rates and a higher rate of chronic kidney disease among post-op patients.3
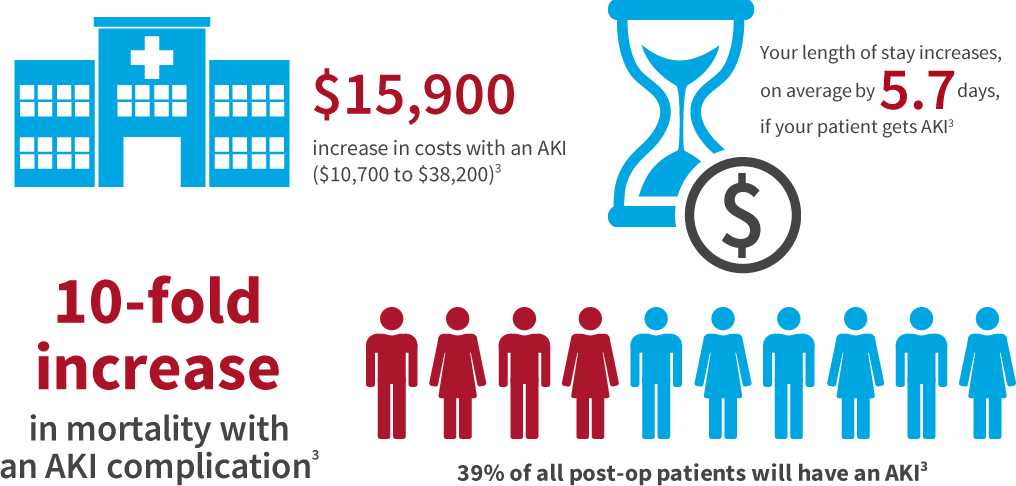
The Challenges of Timely Identification
While a number of acute and patient risk factors have been identified for AKI, there is no reliable way for a clinician to establish a clear risk profile.2
Delays in recognizing acute kidney injury can potentially lead to irreversible consequences,4 but the good news is that in many cases, adverse patient outcomes are avoidable if the condition is recognized and managed in a timely fashion.6
PATIENT RISK FACTORS7
FEMALE
BLACK RACE
CHRONIC KIDNEY DISEASE
CHRONIC DISEASE (HEART, LUNG, LIVER)
DIABETES MELLITUS
CANCER
ANEMIA
DEHYDRATION
ACUTE RISK FACTORS8-11
PNEUMONIA
CARDIOGENIC SHOCK
MAJOR SURGERY
CARDIAC SURGERY
NEPHROTOXIC DRUGS
RADIOCONTRAST AGENTS
HYPOVOLEMIA